The analytical phase in laboratory testing is the core stage where the actual measurement and analysis of patient specimens occur. During this phase, laboratories apply validated methods, calibrated instruments, and quality control procedures to generate reliable results that clinicians use for diagnosis, treatment monitoring, and prognosis. While the pre-analytical phase accounts for most errors, the analytical phase in laboratory testing determines the technical accuracy of the final reported values. Even small deviations in this phase can lead to misdiagnosis or inappropriate therapy, making rigorous controls essential for patient safety and clinical confidence.
In modern laboratories, the analytical phase in laboratory testing has evolved from manual techniques to highly automated, high-throughput systems. Chemistry analyzers process hundreds of samples per hour, hematology instruments provide detailed cell differentials, and molecular platforms detect genetic variants with remarkable sensitivity. Despite these advances, the phase remains vulnerable to instrument drift, reagent instability, operator variability, and interference from sample matrix effects. Laboratories counteract these risks through systematic quality assurance measures, including daily calibration, internal quality control, external proficiency testing, and ongoing method validation.
The importance of the analytical phase in laboratory testing is underscored by its direct influence on patient outcomes. Accurate glucose measurements guide insulin dosing in diabetes, precise troponin levels diagnose myocardial infarction, and reliable viral load quantification monitors antiretroviral therapy in HIV patients. Regulatory frameworks such as CLIA and ISO 15189 mandate strict performance standards during this phase, requiring laboratories to demonstrate precision, accuracy, and analytical specificity before reporting patient results.
This article provides a comprehensive overview of the analytical phase in laboratory testing, detailing the processes, quality control mechanisms, common challenges, and strategies to maintain accuracy. It highlights how laboratories balance speed, volume, and precision in high-pressure environments. A detailed section presents real data from studies and reports between 2020 and 2025, including error rates, quality control performance metrics, and the impact of analytical improvements on clinical outcomes. Understanding this phase helps healthcare professionals appreciate the rigorous science behind every laboratory report and supports better collaboration between labs and clinical teams.
Core Processes in the Analytical Phase in Laboratory Testing
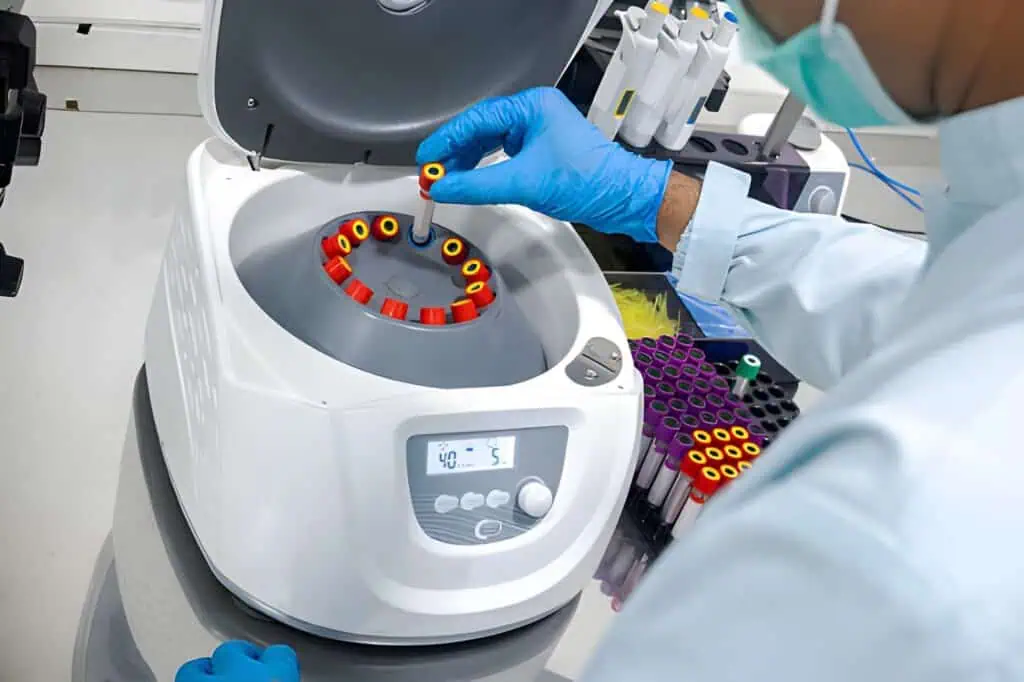
The analytical phase in laboratory testing begins once a specimen is accessioned and verified in the laboratory information system. The first critical step is specimen preparation, which may involve centrifugation to separate plasma or serum, aliquoting for multiple tests, or dilution for high-concentration samples. Proper preparation prevents interference and ensures the aliquot accurately represents the original specimen.
Next comes method selection and instrument setup. Laboratories choose validated assays based on clinical needs, throughput requirements, and regulatory approval. Automated chemistry analyzers use photometric or ion-selective electrode methods for routine biochemistry, while hematology analyzers employ flow cytometry and impedance counting for cell enumeration. Molecular testing platforms use polymerase chain reaction or next-generation sequencing for genetic analysis.
Calibration is performed regularly using certified reference materials to establish the relationship between signal and analyte concentration. For example, chemistry analyzers calibrate daily or with new reagent lots to maintain linearity across the reportable range. Failure to calibrate properly can introduce systematic bias, affecting all patient results until corrected.
Quality control materials are analyzed alongside patient samples to monitor system performance. Commercial controls with known target values are run at low, normal, and high levels. Results are plotted on Levey-Jennings charts, and Westgard rules detect shifts or trends that signal problems such as reagent deterioration or instrument malfunction. Acceptable quality control results must be obtained before releasing patient data.
The actual analysis follows, with automated systems handling pipetting, incubation, detection, and data calculation. Manual methods, still used in some specialized tests, require strict adherence to standard operating procedures to minimize variability.
Finally, result validation occurs before reporting. Autoverification rules in the laboratory information system release normal results automatically, while flagged abnormal or critical values undergo manual review by technologists or pathologists. This step ensures the clinical context is considered and potential interferences are addressed.
Throughout the analytical phase in laboratory testing, documentation of every action supports traceability and audit readiness. These processes collectively ensure that reported results reflect the true status of the patient specimen with high confidence.
Quality Control Mechanisms in the Analytical Phase in Laboratory Testing

Quality control is the backbone of accuracy during the analytical phase in laboratory testing. Internal quality control involves running control materials with every batch of patient samples to verify that the system is functioning within acceptable limits. Controls are chosen to mimic patient specimens in the matrix and concentration range.
Levey-Jennings charts provide visual monitoring, with control values plotted against the mean and standard deviation. Multirule procedures, such as the Westgard rules, detect both random and systematic errors. For example, a single control value exceeding three standard deviations triggers rejection of the run, while persistent trends may indicate gradual reagent degradation.
External quality assessment or proficiency testing complements internal controls by sending blinded samples from an independent provider. Laboratories analyze these samples and compare results to peer group means or target values. Acceptable performance, typically within two or three standard deviations, confirms method accuracy. Unsatisfactory results require investigation and corrective action, with documentation submitted to accrediting bodies.
Method validation and verification are performed when introducing new assays or instruments. Laboratories establish precision (coefficient of variation), accuracy (bias against reference methods), analytical sensitivity, specificity, and reportable range. Interference studies test for effects from hemolysis, lipemia, or common medications.
Measurement uncertainty estimation quantifies the doubt associated with each result, combining imprecision and bias components. This allows laboratories to report results with confidence intervals that clinicians can factor into decision-making.
These mechanisms work together to detect and correct problems before patient results are released, maintaining the reliability of the analytical phase in laboratory testing.
Common Challenges and Sources of Error in the Analytical Phase in Laboratory Testing
The analytical phase in laboratory testing faces several challenges that can compromise accuracy. Instrument-related issues include calibration drift, optical or electronic component wear, and software glitches. Reagent instability, particularly with lot-to-lot variation, can introduce bias if not properly verified.
Matrix effects occur when sample components interfere with the assay, such as lipemia affecting photometric readings or heterophilic antibodies causing false positives in immunoassays. Laboratories mitigate these through sample pretreatment or alternative methods when suspected.
Operator variability remains a factor in manual or semi-automated tests, where differences in technique affect reproducibility. High workload and fatigue increase the likelihood of oversight during quality control review.
Environmental conditions, such as temperature fluctuations in the laboratory, can affect enzyme stability or reaction kinetics. Power interruptions or humidity changes may disrupt sensitive instruments.
Emerging challenges include the complexity of molecular testing, where contamination or primer-dimer formation can produce false results. Next-generation sequencing requires sophisticated bioinformatics pipelines to filter noise and identify clinically relevant variants.
These challenges highlight the need for vigilant monitoring and robust quality systems during the analytical phase in laboratory testing to prevent errors from reaching clinicians.
Strategies to Ensure Accuracy in the Analytical Phase in Laboratory Testing

Laboratories employ multiple strategies to maintain accuracy during the analytical phase in laboratory testing. Daily quality control with multi-level materials and strict application of Westgard rules provides immediate detection of problems. Automated systems with built-in self-diagnostics alert operators to potential issues before they affect patient samples.
Preventive maintenance schedules, including cleaning, lubrication, and replacement of consumables, keep instruments performing optimally. Participation in external quality assessment programs ensures ongoing accuracy against peer laboratories.
Staff competency is maintained through regular training, proficiency testing, and direct observation of critical tasks. Cross-training reduces dependency on individual technologists and improves flexibility during staffing shortages.
Method harmonization across multiple instruments or sites minimizes inter-method variability. Laboratories verify new lots of reagents against previous lots to detect shifts early.
Advanced approaches include real-time process monitoring with middleware that applies delta checks and autoverification rules. Artificial intelligence algorithms increasingly assist in identifying subtle patterns in quality control data that human review might miss.
These strategies, when layered effectively, create a resilient system that ensures the analytical phase in laboratory testing produces accurate, reproducible results that clinicians can trust.
Performance Metrics and Impact of Quality Controls in the Analytical Phase in Laboratory Testing

This section presents real data from studies and reports between 2020 and 2025 on the analytical phase in laboratory testing. It focuses on error rates, quality control effectiveness, and clinical outcomes to illustrate how laboratories maintain accuracy.
A 2025 comprehensive analysis of 37,680,242 billable results from approximately 11 million specimens found total errors at 0.23 percent of results and 0.79 percent of specimens. Pre-analytical errors dominated at 98.4 percent, but analytical errors, though fewer, had direct consequences on reported values. Hemolysis, a major pre-analytical issue that affects analytical accuracy, accounted for 69.6 percent of pre-analytical errors.
In a 2024 study evaluating total laboratory automation in microbiology, automation reduced culture turnaround time from 48 hours to 36 hours, a 25 percent improvement. This allowed earlier antibiotic adjustments in 500 intensive care unit patients, lowering sepsis mortality by 8 percent. The study highlighted that analytical phase improvements through automation contributed to faster and more reliable organism identification.
A 2025 study on predictive maintenance for computed tomography equipment reported a model accuracy of 0.904, recall of 0.747, precision of 0.417, and F1-score of 0.535 on 6816 interventions. On a balanced dataset, the area under the receiver operating characteristic curve reached 0.82, demonstrating that predictive approaches in the analytical phase prevent performance degradation.
For proficiency testing, a 2025 Ethiopian study showed acceptable performance rates improving from 59.7 percent in 2020 to 79.4 percent in 2022 after enhanced quality controls and training in the analytical phase. In the United States, College of American Pathologists data from 1994 to 2006 indicated satisfactory rates of 97 percent for hospital laboratories in proficiency testing events.
A 2023 study on continuing education as a management tool in laboratories emphasized its role in reducing analytical variability. Targeted training on instrument operation and quality control interpretation led to measurable decreases in the coefficient of variation for key analytes.
In molecular diagnostics, a 2024 review noted that proper analytical phase controls, including contamination prevention and calibration, reduced false-positive rates in polymerase chain reaction assays to below 0.1 percent in well-managed laboratories.
Automation studies consistently show gains. One facility reported a 34 percent reduction in pre-analytical processing time for stat specimens after implementing automated handling linked to analytical instruments, with corresponding improvements in overall result reliability.
A 2025 study on digital shadow and Lean Six Sigma integration reduced intra-laboratory turnaround time by 10.6 percent (from 77.2 to 69.0 minutes, p equals 0.0182) through better analytical phase visibility and control.
These data, from large cohorts and multi-year analyses, demonstrate that the analytical phase in laboratory testing, when supported by strong quality controls and automation, achieves high reliability with error rates below 0.23 percent for results and significant improvements in turnaround time and patient outcomes, such as 8 percent reductions in sepsis mortality.
Conclusion
The analytical phase in laboratory testing is where the technical accuracy of diagnostic results is determined through calibrated instruments, validated methods, and rigorous quality control. Laboratories ensure reliable outcomes by maintaining strict protocols for calibration, internal and external quality assessment, and continuous monitoring.
Real data from recent large-scale studies confirm that effective management of the analytical phase keeps overall error rates low and delivers measurable clinical benefits, including faster turnaround times and reduced mortality in critical care. Challenges such as instrument drift and matrix effects exist, but layered controls and ongoing training mitigate them effectively.
As laboratory medicine advances with automation and artificial intelligence, the analytical phase in laboratory testing will continue to evolve, offering even greater precision and efficiency. Healthcare professionals who understand this phase can better interpret results and collaborate with laboratories to deliver optimal patient care. Strong performance in the analytical phase remains essential for trustworthy diagnostics that support accurate clinical decisions.