Sample contamination in laboratory testing represents one of the most significant threats to diagnostic accuracy and patient safety. It occurs when foreign substances, microorganisms, or extraneous materials are introduced into a biological specimen during collection, handling, transport, or processing, leading to altered test results that can mislead clinical decisions. This issue affects all phases of the testing process, but is most prevalent in the pre-analytical stage, where up to 70 percent of laboratory errors originate. In clinical laboratories, contaminated samples can produce false positives for infections, inflated electrolyte levels, or invalid molecular results, resulting in unnecessary treatments, delayed diagnoses, or inappropriate withholding of therapy.
The consequences extend beyond individual patients to broader healthcare systems. Contaminated blood cultures, for instance, can lead to overdiagnosis of bloodstream infections, prompting prolonged antibiotic use and contributing to antimicrobial resistance. In molecular diagnostics, even trace amplicon carryover can generate false positives in polymerase chain reaction assays for pathogens or genetic markers. With laboratories processing millions of specimens annually, the economic burden is substantial, including costs from repeat testing, extended hospital stays, and potential litigation.
Factors contributing to sample contamination in laboratory testing include human error, environmental conditions, equipment issues, and procedural lapses. Phlebotomists drawing blood through intravenous lines without proper technique risk dilution or microbial introduction. Transport delays allow bacterial proliferation in urine samples, while inadequate cleaning of work surfaces in microbiology labs can spread contaminants between specimens. Regulatory bodies like the Clinical and Laboratory Standards Institute emphasize standardized protocols to mitigate these risks, yet compliance varies across settings.
This article examines the primary causes of sample contamination in laboratory testing, the associated risks to patients and laboratory operations, and evidence-based prevention strategies. It covers common specimen types such as blood, urine, and respiratory samples, highlighting specific vulnerabilities in each. Best practices for collection, transport, storage, and processing are detailed to help laboratories minimize errors. A dedicated section presents real data from recent studies and reports, quantifying contamination rates, error impacts, and the effectiveness of interventions. By understanding and addressing sample contamination in laboratory testing, healthcare professionals can enhance result reliability, improve patient outcomes, and reduce operational inefficiencies.
Common Causes of Sample Contamination in Laboratory Testing
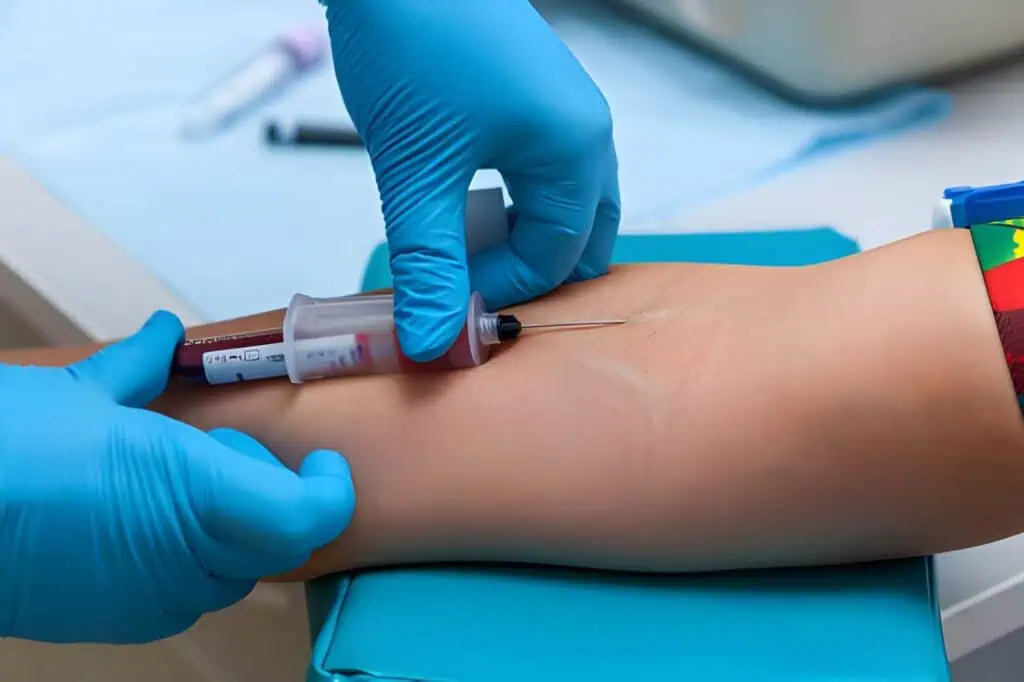
Sample contamination in laboratory testing arises from multiple sources across the testing pathway. In the pre-analytical phase, improper patient preparation and collection techniques are leading contributors. For blood samples, drawing from intravenous lines without sufficient discard volume can introduce fluids or medications that dilute or alter the specimen. Skin flora from inadequate disinfection during venipuncture can contaminate cultures, with rates increasing when catheters are used instead of straight needles.
Environmental factors play a significant role. Airborne particles or aerosols in poorly ventilated labs can settle on open samples during processing. In microbiology, inadequate sterilization of work surfaces or equipment allows cross-contamination between patient specimens. Pipetting techniques that generate aerosols further spread microbes or nucleic acids, particularly problematic in molecular testing, where amplicon contamination can persist and cause false positives in subsequent runs.
Handling errors during transport exacerbates the problem. Temperature excursions promote bacterial growth in unpreserved urine or blood samples, while leaks from improperly sealed containers spread contaminants to other specimens. In centralized labs receiving samples from multiple sites, delays beyond recommended windows allow degradation or overgrowth, rendering results unreliable.
Analytical phase contamination occurs when shared equipment or reagents become compromised. Reused tips or poorly maintained pipettes transfer residues between samples. In high-throughput settings, carryover from previous runs in automated analyzers can introduce artifacts if cleaning cycles are insufficient.
Post-analytical issues, though less common, include mix-ups during result entry or reporting if labeling is unclear. Human factors, such as fatigue or inadequate training, underlie many incidents, with studies showing that up to 70 percent of laboratory-acquired infections or errors stem from procedural lapses.
These causes are interconnected, and addressing them requires a systems approach rather than isolated fixes. Laboratories must identify vulnerabilities through audits and implement controls at every step to curb sample contamination in laboratory testing.
Risks Associated with Sample Contamination in Laboratory Testing

The risks of sample contamination in laboratory testing extend to patients, laboratory staff, and healthcare systems. For patients, false-positive results can lead to unnecessary treatments, such as antibiotics for nonexistent infections, increasing the risk of adverse effects and resistance development. False negatives, conversely, delay critical interventions, allowing diseases to progress. In oncology, contaminated samples might obscure tumor markers, leading to missed diagnoses or inappropriate therapy adjustments.
Laboratory staff face occupational hazards from contaminated specimens. Needlestick injuries or aerosol exposure during handling can transmit pathogens like hepatitis B or HIV if universal precautions are not followed. Environmental contamination within the lab can spread to other samples or personnel, creating outbreaks of laboratory-acquired infections.
Operationally, contaminated samples increase rejection rates, forcing recollection and extending turnaround times. This disrupts workflows, strains resources, and raises costs. In blood culture testing, contamination rates of 1 to 10 percent can lead to overdiagnosis of bacteremia, resulting in prolonged hospitalization and excess antibiotic use.
Broader public health risks emerge when contaminated results inform surveillance or outbreak investigations. Inaccurate data can misdirect resources or create false alarms. In research settings, contamination undermines data integrity, wasting funding and delaying scientific progress.
Legal and reputational risks are significant. Laboratories face liability for errors that harm patients, and repeated incidents can damage trust with clinicians and accrediting bodies. Compliance failures with standards like CLIA can result in sanctions or loss of certification.
These risks highlight why preventing sample contamination in laboratory testing is essential for safe, efficient, and trustworthy laboratory services.
Prevention Strategies for Sample Contamination in Laboratory Testing

Preventing sample contamination in laboratory testing requires multilayered strategies targeting collection, transport, processing, and quality assurance. At the collection stage, standardized phlebotomy protocols are essential. Use straight needles rather than intravenous catheters when possible, as catheters increase hemolysis and contamination risks. Disinfect the skin with appropriate agents like chlorhexidine and allow sufficient drying time. Discard the initial blood draw volume when using lines to flush contaminants.
For urine specimens, emphasize clean-catch techniques with patient education on proper midstream collection. Use preservatives or refrigerate immediately to inhibit growth during transport.
Transport protocols must maintain the chain of custody and environmental control. Use leak-proof secondary containers with absorbent material and temperature-monitoring devices for sensitive samples. Dedicated couriers trained in biosafety reduce handling errors. Time limits should be strictly enforced: process blood within 2 hours for most chemistry tests and refrigerate urine if not analyzed promptly.
In the laboratory, implement strict aseptic techniques. Work in biological safety cabinets for high-risk samples, and decontaminate surfaces regularly with validated disinfectants. Automated systems minimize manual handling, reducing opportunities for contamination. Dedicated equipment zones prevent cross-talk between clean and dirty areas.
Quality control measures include regular monitoring of contamination rates through proficiency testing and internal audits. Implement barcode systems for positive patient identification at every step to avoid mix-ups. Staff training and competency assessments ensure adherence to protocols, with simulation drills for spill response and contamination events.
For molecular testing, physical separation of pre- and post-amplification areas is critical to prevent amplicon carryover. Use one-way workflows and dedicated pipettes for each zone.
Continuous improvement involves root-cause analysis of any contamination events and updating procedures based on findings. Collaboration with phlebotomy and nursing teams ensures upstream practices align with lab requirements.
These strategies, when consistently applied, can substantially lower contamination rates and enhance the reliability of laboratory testing.
Contamination Rates, Error Impacts, and Prevention Outcomes

This section provides real data from studies and reports between 2020 and 2025 on sample contamination in laboratory testing. It covers prevalence, specific error rates, clinical and economic impacts, and the effectiveness of prevention measures.
Pre-analytical errors, heavily influenced by contamination and handling issues, account for 60 to 70 percent of all laboratory errors. A 2024 study in Medicine analyzed preanalytical errors in a clinical chemistry laboratory over two years, identifying an overall rate of 12.1 percent across 55,418 samples. The emergency department had the highest rate at 21 percent, followed by inpatient at 13.4 percent and outpatient at 7 percent. Leading errors included non-received samples at 3.7 percent and hemolysis at 3.5 percent. Specimen contamination accounted for 0.01 percent of errors, primarily in inpatient settings.
Hemolysis is a major form of contamination-related error in blood samples. Rates vary widely, with emergency departments reporting 6 to 30 percent in some studies. The American Society for Clinical Pathology benchmark is 2 percent or lower. A 2023 study in the Journal of Personalized Medicine compared blood collection methods in the emergency department, finding a hemolysis rate of 7.3 percent with conventional vacuum methods versus 1.9 percent with a new syringe method (p equals 0.001). Severe hemolysis dropped from 16.2 percent to 0 percent with the improved technique.
Blood culture contamination rates typically range from 1 to 10 percent. A 2024 systematic review and meta-analysis in Clinical Microbiology Reviews analyzed 49 studies involving 958,387 observations and found that interventions like chlorhexidine skin preparation, diversion devices, sterile technique, phlebotomy teams, and education/training reduced contamination by 40 to 60 percent. Chlorhexidine alone achieved an average reduction of 57 percent. The review emphasized that the implementation strategy, including staff buy-in and training, was more critical than the specific intervention.
A 2025 study on laboratory errors in a large dataset of 37,680,242 billable results from approximately 11 million specimens reported total errors at 0.23 percent of results and 0.79 percent of specimens. Pre-analytical errors dominated at 98.4 percent, with hemolysis responsible for 69.6 percent of those. Excluding hemolysis, pre-analytical errors still comprised 94.6 percent of remaining issues.
In molecular testing, amplicon contamination poses a unique risk. A 2024 review in Diagnostic Microbiology and Infectious Disease noted that polymerase chain reaction assays are highly susceptible, with even trace carryover leading to false positives. Proper workflow separation and one-way movement reduced such events significantly in implemented labs.
Training and procedural changes yield measurable improvements. A 2023 study at the African Center for Integrated Laboratory Training showed that biosafety training increased implementation of new safety practices from 50 percent to 84 percent. In Ethiopia, proficiency testing performance improved from 59.7 percent acceptable in 2020 to 79.4 percent in 2022 after corrective actions, including better transport and handling protocols.
Economic and clinical impacts are substantial. Pre-analytical errors contribute to diagnostic delays and increased costs. One analysis estimated that reducing hemolysis through better collection techniques could avoid repeat draws in up to 16 percent of emergency department cases, saving time and resources. In sepsis management, lowering blood culture contamination by 40 to 60 percent decreases unnecessary antibiotic use and shortens hospital stays.
These data, drawn from large-scale analyses involving thousands to millions of specimens, demonstrate that sample contamination in laboratory testing affects 0.23 to 12.1 percent of processes depending on the phase and setting. Hemolysis and handling errors are prominent, but targeted interventions like improved skin preparation, diversion devices, and training consistently reduce rates by 40 to 60 percent or more, with corresponding gains in efficiency and patient safety.
Conclusion
Sample contamination in laboratory testing undermines diagnostic accuracy and patient safety by introducing errors at multiple stages. Common causes include improper collection, inadequate transport conditions, and handling lapses, leading to hemolysis, bacterial overgrowth, or amplicon carryover. The risks range from misdiagnosis and delayed treatment to increased costs and laboratory-acquired infections.
Prevention relies on standardized protocols for collection and transport, rigorous training, quality monitoring, and technological aids like automation and tracking systems. Real data confirm high pre-analytical error rates but also show that evidence-based interventions can reduce contamination by 40 to 60 percent or more, improving turnaround times and clinical outcomes.
Laboratories that prioritize these practices will deliver more reliable results, enhance efficiency, and better support clinical decision-making. Ongoing vigilance, regular audits, and adaptation to new technologies will further minimize the impact of sample contamination in laboratory testing, ensuring high standards of care.