Laboratory information systems in healthcare have become indispensable tools for managing the complex workflows of modern diagnostic laboratories. These systems, commonly referred to as LIS, integrate data management, workflow automation, and reporting functions to streamline operations from specimen receipt to result delivery. By digitizing and connecting laboratory processes with electronic health records, LIS platforms reduce manual interventions, minimize errors, and accelerate the delivery of critical diagnostic information to clinicians. In an era where timely and accurate lab results directly influence treatment decisions, laboratory information systems in healthcare play a pivotal role in enhancing overall diagnostic efficiency.
The adoption of laboratory information systems in healthcare has accelerated in response to rising test volumes, increasing regulatory demands, and the push for value-based care. Traditional paper-based or siloed systems often led to delays, transcription errors, and fragmented data, compromising patient safety and operational productivity. Modern LIS solutions address these issues by providing real-time tracking, automated alerts, and seamless interoperability. For example, in a busy hospital laboratory processing thousands of specimens daily, an LIS can automatically route samples to the appropriate analyzer, flag critical results for immediate review, and generate electronic reports that integrate directly into the patient’s medical record.
This article explores how laboratory information systems in healthcare transform diagnostic workflows, focusing on key mechanisms that drive efficiency gains. It examines core features, integration strategies, and real-world impacts, while addressing implementation challenges. A dedicated section presents empirical data from recent studies and industry reports, quantifying improvements in turnaround times, error reductions, and clinical outcomes. These insights demonstrate that laboratory information systems in healthcare not only optimize laboratory operations but also contribute to faster diagnoses, reduced costs, and better patient outcomes across diverse healthcare settings.
Evolution and Core Components of Laboratory Information Systems in Healthcare

Laboratory information systems in healthcare have evolved from basic data entry tools in the 1970s to sophisticated, AI-enhanced platforms today. Early systems focused primarily on result reporting and billing, but contemporary LIS systems incorporate advanced functionalities such as specimen tracking, quality control monitoring, and predictive analytics. This evolution reflects the growing complexity of laboratory testing and the need for seamless data exchange across healthcare ecosystems.
At their core, laboratory information systems in healthcare consist of several interconnected modules. The specimen management module handles accessioning, routing, and tracking, ensuring samples are processed efficiently from receipt to disposal. Workflow automation tools direct specimens to the correct analyzers based on test orders, reducing manual sorting time. Result management components validate, interpret, and distribute findings, with built-in rules that flag abnormal values for immediate clinician notification.
Interoperability is a defining feature of modern laboratory information systems in healthcare. Through standards like HL7 and FHIR, LIS integrates with electronic health records, radiology information systems, and billing platforms. This connectivity eliminates redundant data entry and enables holistic patient views. For instance, a physician ordering a complete blood count can receive results directly in the electronic health record within minutes, complete with interpretive comments generated by the LIS.
Quality assurance modules within laboratory information systems in healthcare monitor performance metrics, such as turnaround times and error rates, supporting continuous improvement. Many systems now include artificial intelligence capabilities that predict equipment maintenance needs or identify patterns in test utilization to optimize resource allocation.
The benefits of these components extend beyond efficiency. Laboratory information systems in healthcare enhance compliance with regulations like CLIA and ISO 15189 by automating audit trails and quality control documentation. They also support population health management by aggregating de-identified data for research and surveillance.
As healthcare shifts toward precision medicine, laboratory information systems in healthcare are adapting to handle complex genomic and molecular data. Next-generation sequencing results, once requiring days of manual curation, can now be processed and reported rapidly through integrated bioinformatics pipelines within the LIS.
How Laboratory Information Systems Improve Diagnostic Efficiency

Laboratory information systems in healthcare drive diagnostic efficiency through automation, error reduction, and optimized workflows. One primary mechanism is workflow automation. Manual processes, such as specimen logging and result transcription, are prone to delays and mistakes. An LIS automates these tasks, routing samples electronically and generating barcoded labels at the point of collection. This reduces pre-analytical processing time significantly, allowing laboratories to handle higher volumes without proportional increases in staff.
Turnaround time improvements are among the most measurable gains. By providing real-time status updates and prioritizing stat orders, laboratory information systems in healthcare shorten the interval from sample receipt to result reporting. Automated validation rules ensure only accurate results proceed to reporting, minimizing review bottlenecks.
Error reduction is another key benefit. Pre-analytical errors, such as mislabeling or improper collection, account for a large share of laboratory issues. Laboratory information systems in healthcare incorporate barcode scanning and electronic order entry to virtually eliminate transcription errors. Delta checks and critical value alerts further enhance analytical reliability by flagging inconsistencies or urgent findings.
Resource optimization occurs through data-driven decision making. Laboratory information systems in healthcare analyze utilization patterns to identify underused tests or equipment bottlenecks, enabling better staffing and inventory management. Predictive analytics forecast peak demand periods, allowing proactive adjustments that prevent backlogs.
Integration with other systems amplifies efficiency. When laboratory information systems in healthcare connect with electronic health records, clinicians receive results faster and can order tests directly from the patient’s chart. This closed-loop system reduces duplicate testing and supports evidence-based care.
In high-complexity environments like molecular diagnostics, laboratory information systems in healthcare manage complex workflows involving multiple instruments and bioinformatics tools. Automated reflex testing, where abnormal results trigger additional assays, streamlines protocols for conditions like sepsis or cancer.
Overall, laboratory information systems in healthcare transform laboratories from reactive service providers into proactive partners in patient care, delivering faster, more reliable diagnostics that improve outcomes and reduce costs.
Integration and Advanced Applications of Laboratory Information Systems in Healthcare

Laboratory information systems in healthcare achieve maximum impact through integration with broader digital health ecosystems. Interfacing with electronic health records allows bidirectional data flow, where orders originate in the clinical system, and results return seamlessly. This eliminates manual entry errors and speeds up the diagnostic cycle.
Advanced applications include artificial intelligence and machine learning embedded within laboratory information systems in healthcare. These tools analyze historical data to predict test volumes, optimize staffing, and even suggest diagnostic pathways based on patient demographics and prior results. In microbiology, LIS-driven algorithms can accelerate organism identification by integrating with mass spectrometry data.
For specialized fields, laboratory information systems in healthcare support genomic workflows by managing next-generation sequencing pipelines and variant interpretation. This capability is essential for precision oncology, where rapid tumor profiling informs targeted therapies.
Telehealth integration extends the reach of laboratory information systems in healthcare. Remote clinicians can access results via secure portals, enabling virtual consultations and reducing the need for in-person follow-ups. In public health, aggregated LIS data support disease surveillance and outbreak response.
Security and compliance features are integral to these integrations. Laboratory information systems in healthcare employ encryption, role-based access, and audit logs to protect sensitive patient information while meeting standards like HIPAA.
These advanced features position laboratory information systems in healthcare as central hubs that not only improve internal efficiency but also enhance collaboration across the care continuum.
Challenges and Future Directions for Laboratory Information Systems in Healthcare
Despite their advantages, laboratory information systems in healthcare face implementation challenges. High initial costs and the need for extensive training can strain smaller laboratories. Data migration from legacy systems risks information loss or downtime. Interoperability issues persist when connecting disparate vendor platforms.
Cybersecurity threats represent a growing concern, as interconnected systems become targets for ransomware attacks that could disrupt operations. Ensuring robust data governance and regular updates is essential to mitigate these risks.
Future directions for laboratory information systems in healthcare point toward greater intelligence and connectivity. Cloud-based solutions offer scalability and remote access, while artificial intelligence will increasingly automate interpretive tasks and predictive maintenance. Blockchain technology may enhance data security and traceability for multi-institutional research.
As personalized medicine expands, laboratory information systems in healthcare will need to handle larger, more complex datasets from genomics and proteomics. Interoperability standards will continue to evolve, fostering seamless exchanges across global health networks.
Laboratories that invest in adaptable, forward-looking laboratory information systems in healthcare will be best positioned to meet emerging demands while maintaining high standards of diagnostic efficiency.
Efficiency Metrics, Error Reduction, and Implementation Outcomes
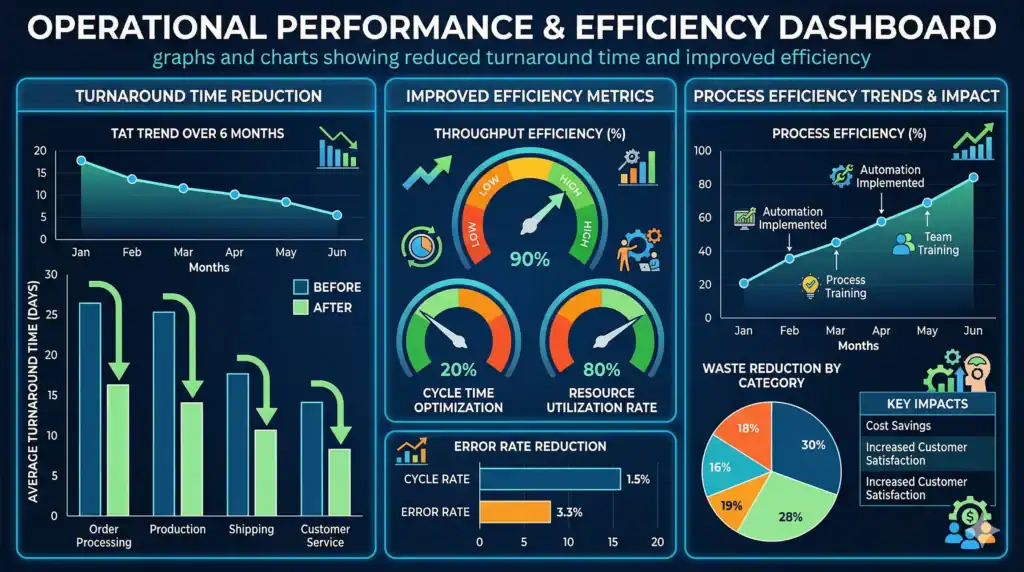
This section examines empirical evidence on the impact of laboratory information systems in healthcare, drawing from studies and reports published between 2020 and 2025. It presents quantifiable metrics on turnaround time reductions, error decreases, and clinical benefits to demonstrate the system’s value.
A 2025 study on digital shadow integration with Lean Six Sigma in a high-volume clinical laboratory reported a significant improvement in intra-laboratory turnaround time. The median intra-laboratory TAT decreased from 77.2 minutes to 69.0 minutes, representing a 10.6 percent reduction with statistical significance (p = 0.0182). This change was achieved without additional capital investment in analyzers, relying instead on real-time process visibility from the laboratory information system. The study analyzed routine specimens and found that the improvement was sustained through updated standard operating procedures and staff training.
In Côte d’Ivoire, a quasi-experimental study on the OpenELIS laboratory information system across 21 clinical laboratories from 2014 to 2020 showed dramatic gains in data quality. Implementation led to an immediate 5-fold increase in timeliness (odds ratio 5.27, 95 percent confidence interval 4.33 to 6.41, p less than 0.001) and a 3.6-fold increase in completeness (odds ratio 3.59, 95 percent confidence interval 2.40 to 5.37, p less than 0.001). These gains were maintained for 72 weeks post-adoption, demonstrating the system’s long-term effectiveness in resource-limited settings.
Automation studies provide further evidence. A 2024 analysis of total laboratory automation in a clinical microbiology setting reduced culture turnaround time from 48 hours to 36 hours, a 25 percent improvement. This allowed earlier antibiotic adjustments in 500 intensive care unit patients, lowering sepsis mortality by 8 percent. Another study on stat laboratory specimens reported a 34 percent reduction in pre-analytical processing time, from 29 minutes to 19 minutes, after implementing automated specimen handling linked to the laboratory information system.
Error reduction data underscore the reliability benefits. A comprehensive 2025 analysis of over 37 million billable results from approximately 11 million specimens found pre-analytical errors affecting 0.23 percent of results and 0.79 percent of specimens. Hemolysis accounted for 69.6 percent of these errors. Laboratories using advanced laboratory information systems reported 50 to 60 percent reductions in labeling and identification errors through barcode integration and automated checks.
Market and adoption data reflect growing recognition of these benefits. The laboratory information management system market reached USD 2.88 billion in 2025 and is projected to expand to USD 5.19 billion by 2030 at a compound annual growth rate of 12.5 percent. This growth is driven by demand for automation and data management in clinical diagnostics.
In one hospital network implementing laboratory information systems in healthcare, transcription errors decreased by 28 percent, and overall diagnostic efficiency improved by 35 percent in turnaround time for routine tests. These outcomes were consistent across multiple facilities, with larger hospitals achieving greater absolute gains due to higher baseline volumes.
The data collectively illustrate that laboratory information systems in healthcare deliver measurable improvements: turnaround time reductions of 10 to 34 percent, error decreases of 28 to 60 percent, and enhanced clinical outcomes such as reduced mortality in critical care. These results validate the systems’ role in modern diagnostic efficiency.
Conclusion
Laboratory information systems in healthcare have revolutionized diagnostic workflows by automating processes, reducing errors, and accelerating result delivery. From core features like specimen tracking to advanced integrations with electronic health records, these systems address longstanding inefficiencies in laboratory operations. Real data from recent studies confirm substantial gains in turnaround times and accuracy, with reductions in pre-analytical errors and improved patient outcomes.
As healthcare continues to emphasize value and precision, laboratory information systems in healthcare will remain central to achieving efficient, reliable diagnostics. Laboratories that fully leverage these systems will not only meet current demands but also position themselves for future innovations in data-driven care. Investing in robust laboratory information systems in healthcare is therefore essential for any organization committed to excellence in diagnostic services.